Introduction
Understanding the relationship between hormonal imbalances and headaches can feel overwhelming, yet it’s crucial for women’s health. Many women experience debilitating headaches, particularly migraines, during significant life phases when hormones like estrogen and progesterone fluctuate. This connection can leave you feeling frustrated and helpless.
But there’s hope. This article explores how these hormonal changes can trigger specific types of headaches and offers effective solutions and treatment options. By uncovering these nuances, we can better understand how hormonal influences stack up against other common headache triggers.
What’s more, we’ll discuss personalized strategies that can help alleviate discomfort and empower you to regain control over your well-being. You’re not alone in this journey, and together, we can find the right path to relief.
Understand Hormonal Imbalances and Their Role in Headaches
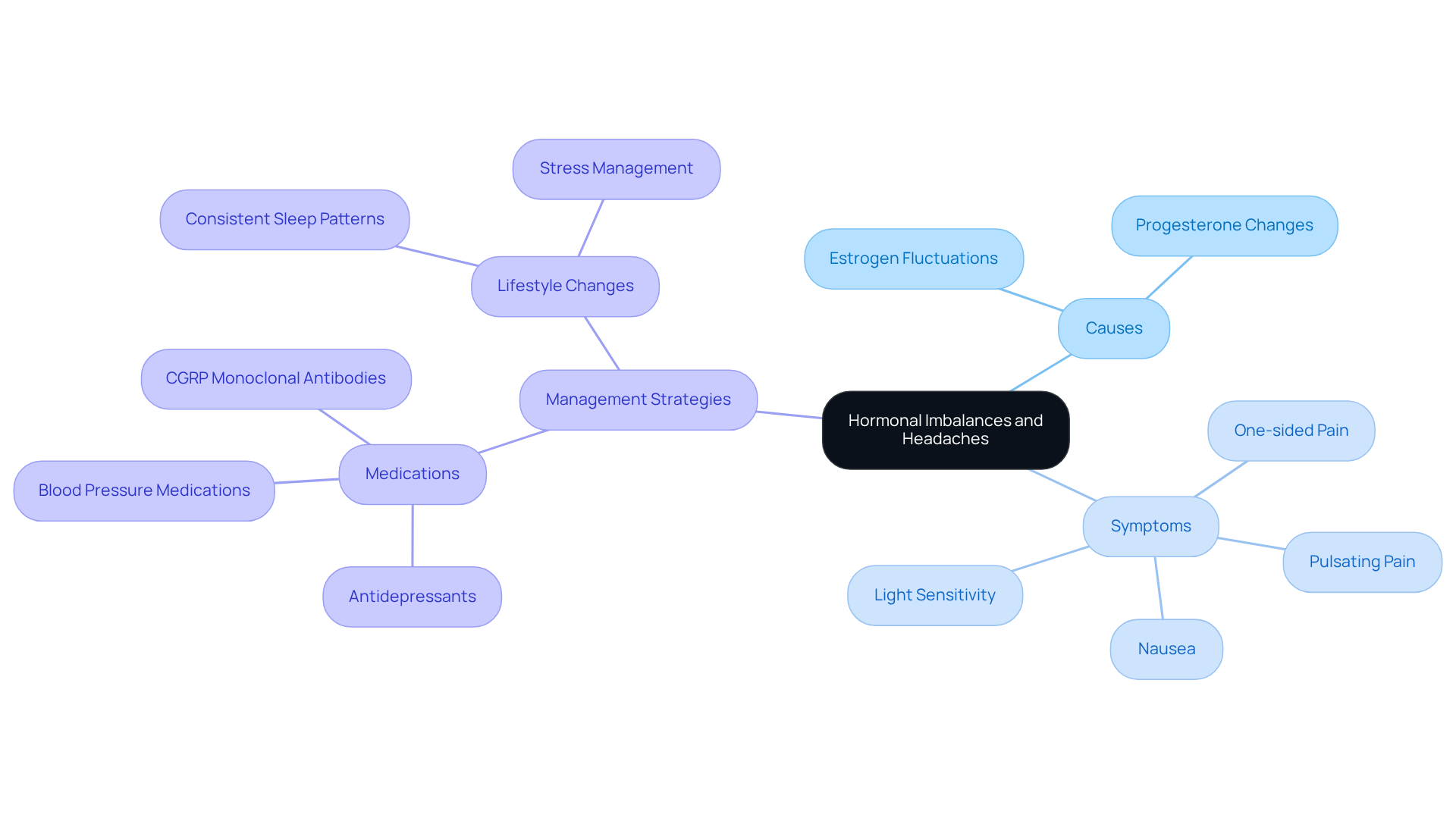
Many women wonder if a can cause headaches, particularly due to that can significantly affect their health. Many women find that a drop in estrogen levels, which frequently happens before menstruation, raises the question of whether a can cause headaches. This is a common experience; research shows that numerous women notice an during their menstrual cycles, leading to the question of whether a hormone imbalance can cause headaches due to these hormonal changes. is crucial for recognizing the unique features of , which often present as one-sided, pulsating pain accompanied by nausea and light sensitivity. This is different from other types of headaches, which may not have such a clear hormonal link.
If you’re a woman considering , it’s important to consult with a primary care provider or gynecologist. Some contraceptives can increase stroke risk, particularly in women who experience headaches with aura. Thankfully, there are , such as:
- antidepressants
- blood pressure medications
- CGRP monoclonal antibodies
that can help manage .
Additionally, maintaining consistent sleep patterns and managing stress levels are essential strategies for reducing headache frequency. As neurologist Sasikanth Gorantla points out, "Our findings show that even a small disruption to the body’s internal clock can have an impact on people living with migraines." This highlights the importance of addressing biological factors in effective . Remember, you’re not alone in this, and there are supportive solutions available to help you navigate these challenges.
Identify Other Common Headache Triggers
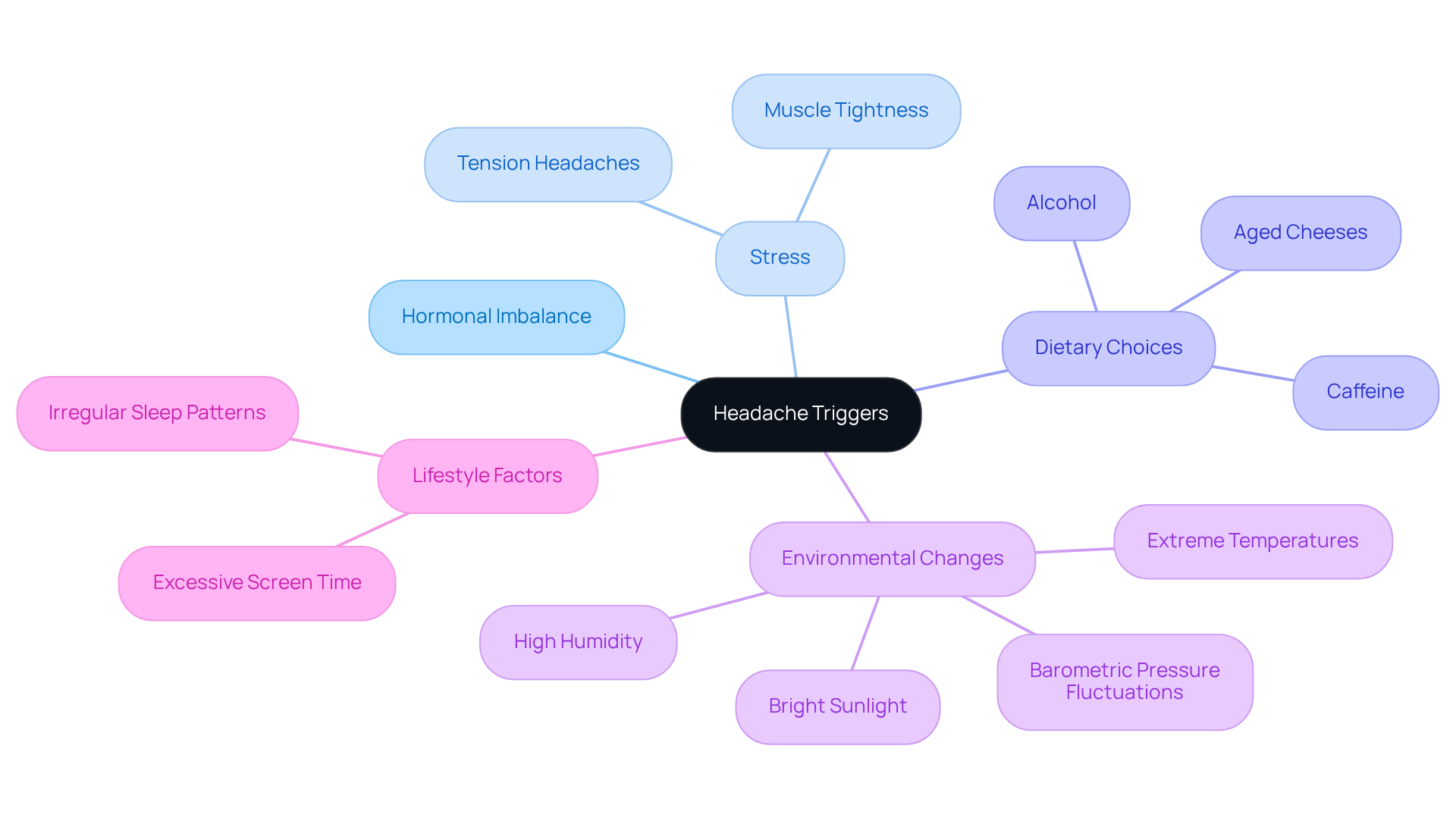
Headaches can often feel overwhelming, and it raises the question: can a cause headaches among the various triggers? Stress, dehydration, dietary choices, and even can all play a role in your discomfort. For example, tension headaches are frequently linked to , while migraines can be aggravated by certain foods like aged cheeses or alcohol.
Dr. Emad Estemalik, a specialist at the Cleveland Clinic, highlights the importance of managing stress and being mindful of environmental factors to alleviate discomfort. Additionally, lifestyle choices such as irregular sleep patterns and excessive screen time can contribute to the frequency of headaches. Understanding these triggers is vital for anyone who experiences discomfort, as it allows for a more to prevention and care.
Recent studies have shown that fluctuations in barometric pressure and can significantly affect . This underscores the need to stay aware of . Having on hand during shifts in weather can be a proactive step in . However, it’s essential to be cautious about overusing , as this can lead to rebound headaches, complicating the management of migraine conditions. By recognizing these factors and taking thoughtful steps, you can find relief and regain control over your well-being.
Compare Treatment Options for Hormonal vs. Other Headache Causes
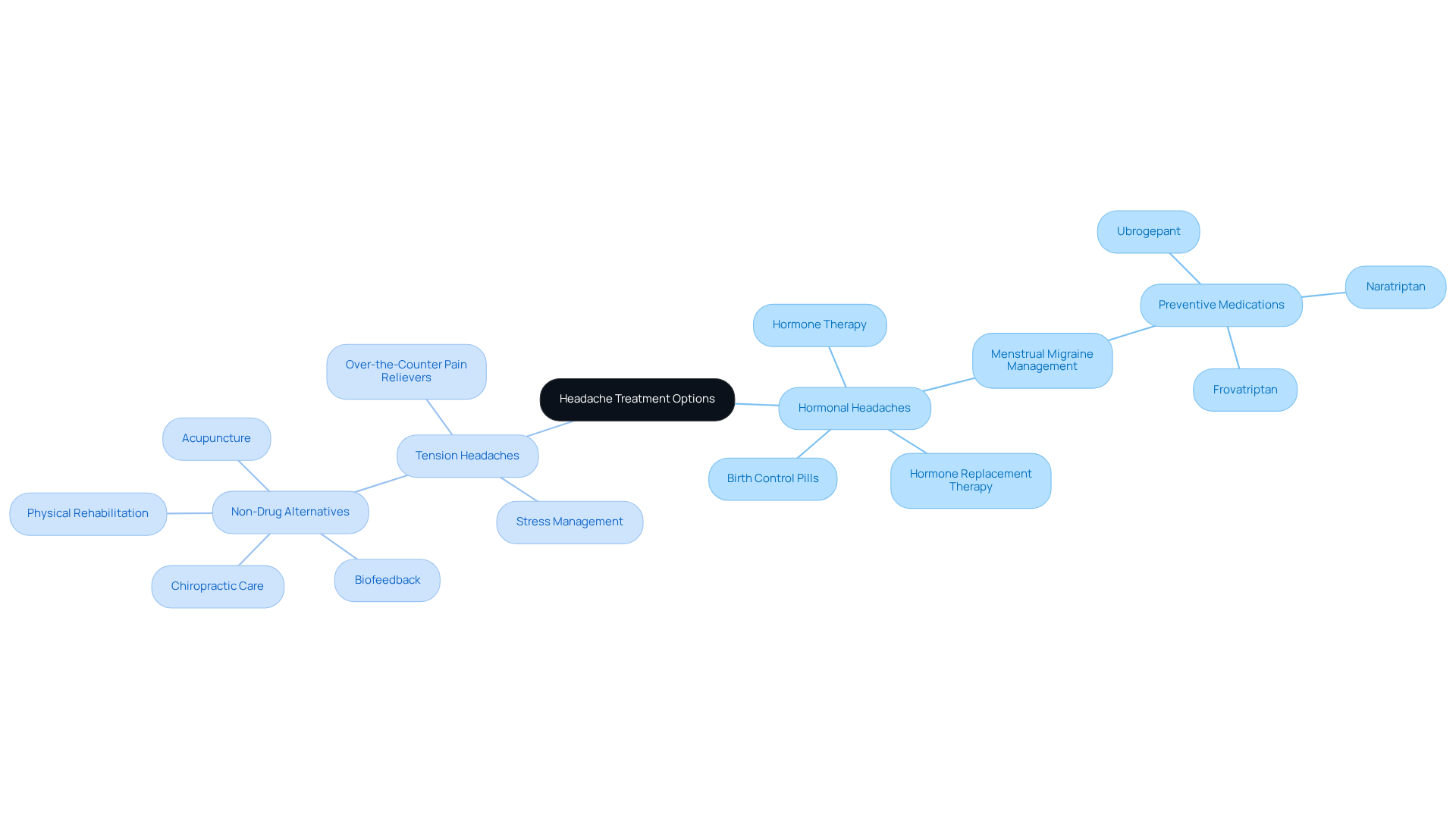
Migraines can be a significant challenge, often stemming from various root causes. For many women, the question of whether a is significant, as . Hormone-related discomfort can often be alleviated through effective remedies like , including birth control pills or hormone replacement therapy. These treatments aim to stabilize estrogen levels, which can help reduce the frequency and severity of headaches. Research shows that , raise the question of whether a , as they can lead to who suffer from migraines.
On the other hand, , stress management techniques, and lifestyle changes. At Innovative Medicine, our healthcare experts emphasize the importance of . Tension discomfort may respond well to non-drug alternatives such as:
- acupuncture
- chiropractic care
- physical rehabilitation
- biofeedback
These approaches can provide significant relief and support overall well-being.
Recent advancements in endocrine treatment are also promising. show potential for improving migraine management in women. Many patients have reported substantial relief from endocrine pain through customized interventions, highlighting the effectiveness of these .
Understanding the differences in is essential for anyone seeking the most suitable strategy for their specific type of pain. By exploring these alternatives, individuals can find the support and relief they need to manage their migraines effectively.
Summarize Key Differences Between Hormonal and Other Headache Triggers
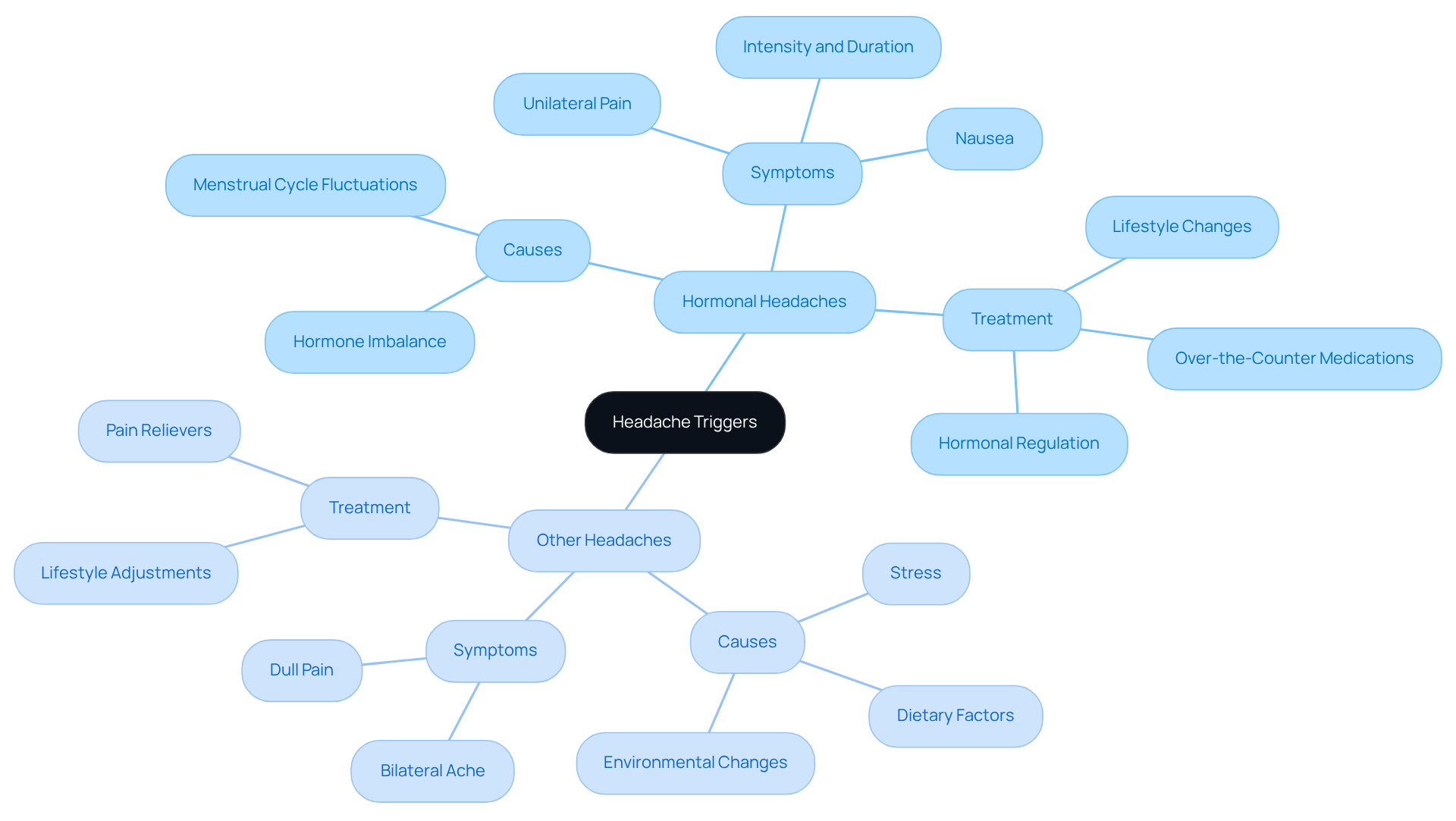
A significant challenge posed by hormonal headaches raises the question: can a cause headaches, primarily influenced by fluctuations in estrogen and progesterone? These headaches often correlate with menstrual cycles, raising the question of whether a can cause headaches, making them a common concern for many women. While other headache types may arise from various triggers - like stress, dietary factors, and environmental changes - have their own distinct characteristics. They typically present with , which can be quite distressing. In contrast, tension-related discomfort often manifests as a dull, bilateral ache, which, while uncomfortable, may not carry the same intensity.
It's important to recognize that raise the question of whether a hormone imbalance can cause headaches, affecting about 50% to 60% of women who experience headaches. These headaches can be more intense and last longer than those occurring at other times, adding to the emotional toll they can take. Understanding this can help in acknowledging the struggle many face, and it’s crucial to approach this issue with compassion and support.
When it comes to treatment, strategies can vary significantly. often require , which can feel daunting. However, there are also that can provide relief for other types of discomfort. As Dr. Murali Chekuri wisely notes, 'Estrogen acts as a primary hormone that initiates headache episodes.' This insight underscores the importance of recognizing the unique nature of hormonal headaches.
By understanding these differences, you can take proactive steps toward . Identifying and avoiding personal migraine triggers is essential, and knowing that support and solutions are available can bring comfort and reassurance.
Conclusion
Understanding the connection between hormonal imbalances and headaches is vital for finding effective relief. For many, especially women, fluctuations in hormones like estrogen and progesterone can trigger migraines. By recognizing that these headaches often align with menstrual cycles, individuals can pinpoint their triggers and pursue tailored treatments that meet their unique needs.
This article sheds light on various factors that contribute to headaches, such as stress, dietary habits, and environmental influences, alongside hormonal changes. It underscores the significance of personalized treatment strategies - whether through hormonal therapies for hormone-related migraines or lifestyle changes for tension headaches. By distinguishing between these headache types, individuals can take informed steps toward alleviating discomfort and enhancing their overall well-being.
In conclusion, being aware of how hormonal imbalances can lead to headaches is crucial for those affected. By grasping the unique traits of hormonal migraines and the range of treatment options available, individuals can empower themselves to seek effective solutions. A proactive approach, which includes lifestyle adjustments and consultations with healthcare professionals, can greatly improve quality of life and provide relief from the burden of headaches.
Frequently Asked Questions
Can hormonal imbalances cause headaches in women?
Yes, hormonal imbalances, particularly fluctuations in estrogen and progesterone, can lead to headaches. Many women experience an increase in migraine frequency during their menstrual cycles, often linked to drops in estrogen levels.
What are the characteristics of hormone-related migraines?
Hormone-related migraines typically present as one-sided, pulsating pain accompanied by nausea and light sensitivity, distinguishing them from other types of headaches that may not have a clear hormonal link.
Should women considering birth control for headache management consult a healthcare provider?
Yes, it is important for women to consult with a primary care provider or gynecologist when considering birth control options for headache management, as some contraceptives can increase stroke risk, especially in women with headaches that have aura.
What types of medications are available for managing headaches related to hormonal changes?
Preventive medications for managing headaches related to hormonal changes include antidepressants, blood pressure medications, and CGRP monoclonal antibodies.
What lifestyle strategies can help reduce headache frequency?
Maintaining consistent sleep patterns and managing stress levels are essential strategies for reducing headache frequency.
How does disruption to the body's internal clock affect migraines?
A small disruption to the body’s internal clock can impact individuals living with migraines, highlighting the importance of addressing biological factors in effective pain management.




