Introduction
Navigating the complexities of hormonal imbalances, especially during menopause, can be challenging for many women. Understanding the differences between Bioidentical Hormone Replacement Therapy (BHRT) and traditional Hormone Replacement Therapy (HRT) is crucial in this journey. Each therapy presents unique approaches to alleviating symptoms, with BHRT utilizing hormones that closely mimic the body’s natural chemistry. This can lead to more effective and personalized care, offering hope to those seeking relief.
As discussions around hormonal treatments evolve, it’s natural to have questions about safety, effectiveness, and individual health needs. Many women find themselves wondering which option truly aligns with their unique health journey. This uncertainty can be overwhelming, but it’s important to remember that you’re not alone. With the right information and support, you can make informed decisions that prioritize your well-being.
Define BHRT and HRT: Core Differences
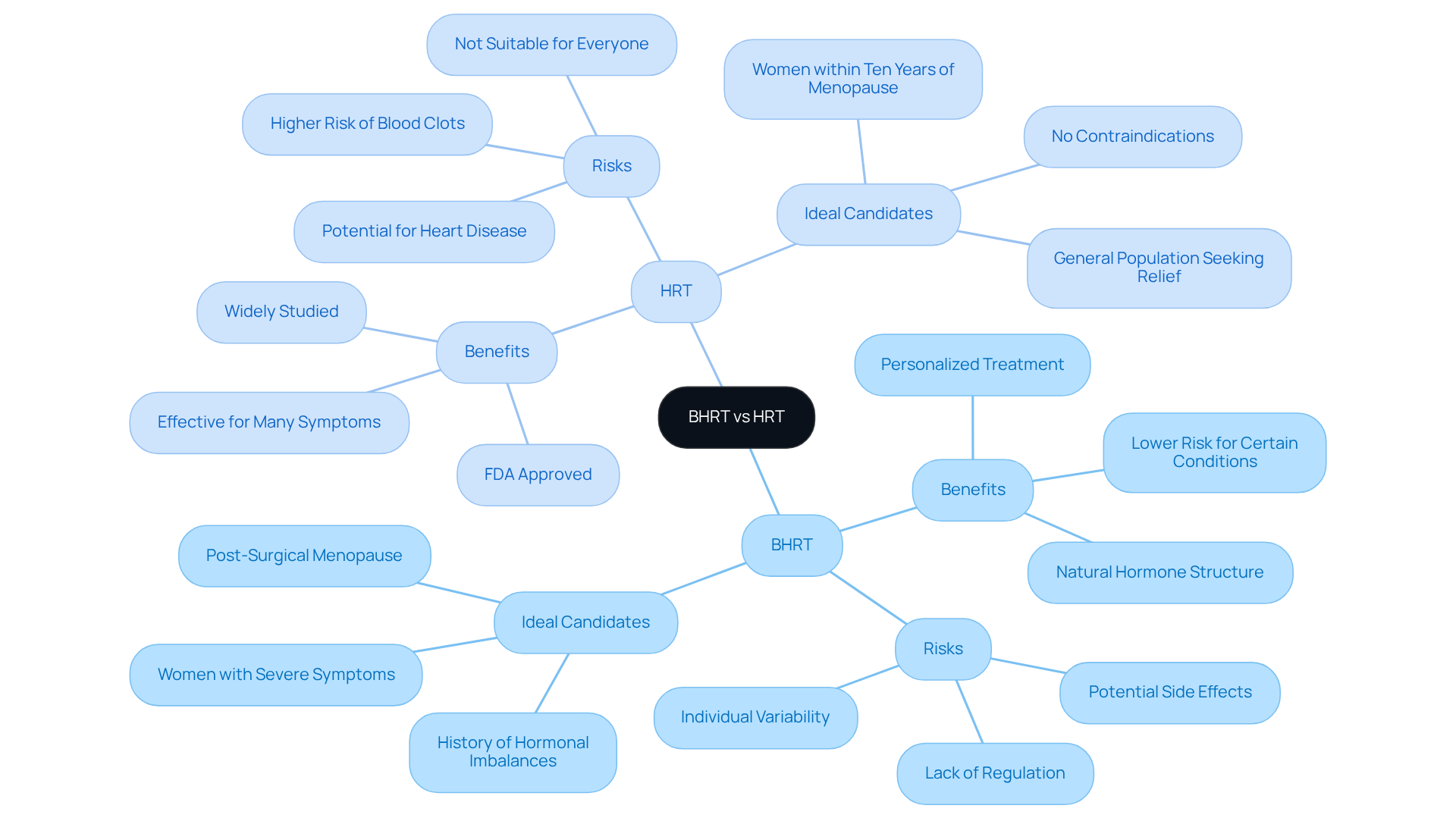
Bioidentical Hormone Replacement Therapy (BHRT) and Hormone Replacement Therapy (HRT) are designed to alleviate the discomfort associated with hormonal imbalances, highlighting the differences in BHRT vs HRT, particularly during menopause. Many women experience a range of symptoms during this time, and it can feel overwhelming. BHRT uses substances that are chemically identical to those naturally produced by the body, like estradiol and progesterone, which are derived from plants. This similarity allows BHRT to work harmoniously with your body’s own hormonal chemistry, potentially offering more effective relief with fewer side effects.
On the other hand, traditional HRT often relies on synthetic substances or those sourced from animals, which may not match the body’s natural hormones as closely. This difference in chemical composition can significantly influence how each treatment interacts with your body. Recent studies suggest that bioidentical substances, especially transdermal estradiol combined with micronized progesterone, may present a safer option compared to synthetic alternatives highlighted in the Women’s Health Initiative (WHI).
Moreover, research indicates that starting hormonal treatment early can reduce the risk of osteoporosis and fractures in postmenopausal women. Those who begin HRT shortly after menopause may experience a 13% lower risk of fractures compared to those who do not use HRT. This underscores the importance of timely intervention and the in managing menopausal symptoms effectively.
As conversations around hormonal treatments evolve, it’s crucial for women to consider the differences in BHRT vs HRT, particularly in terms of safety, effectiveness, and individual health needs. Engaging with knowledgeable healthcare providers can ensure that treatment plans are customized to fit each woman’s unique physiology and health objectives.
Evaluate Benefits and Risks of BHRT and HRT
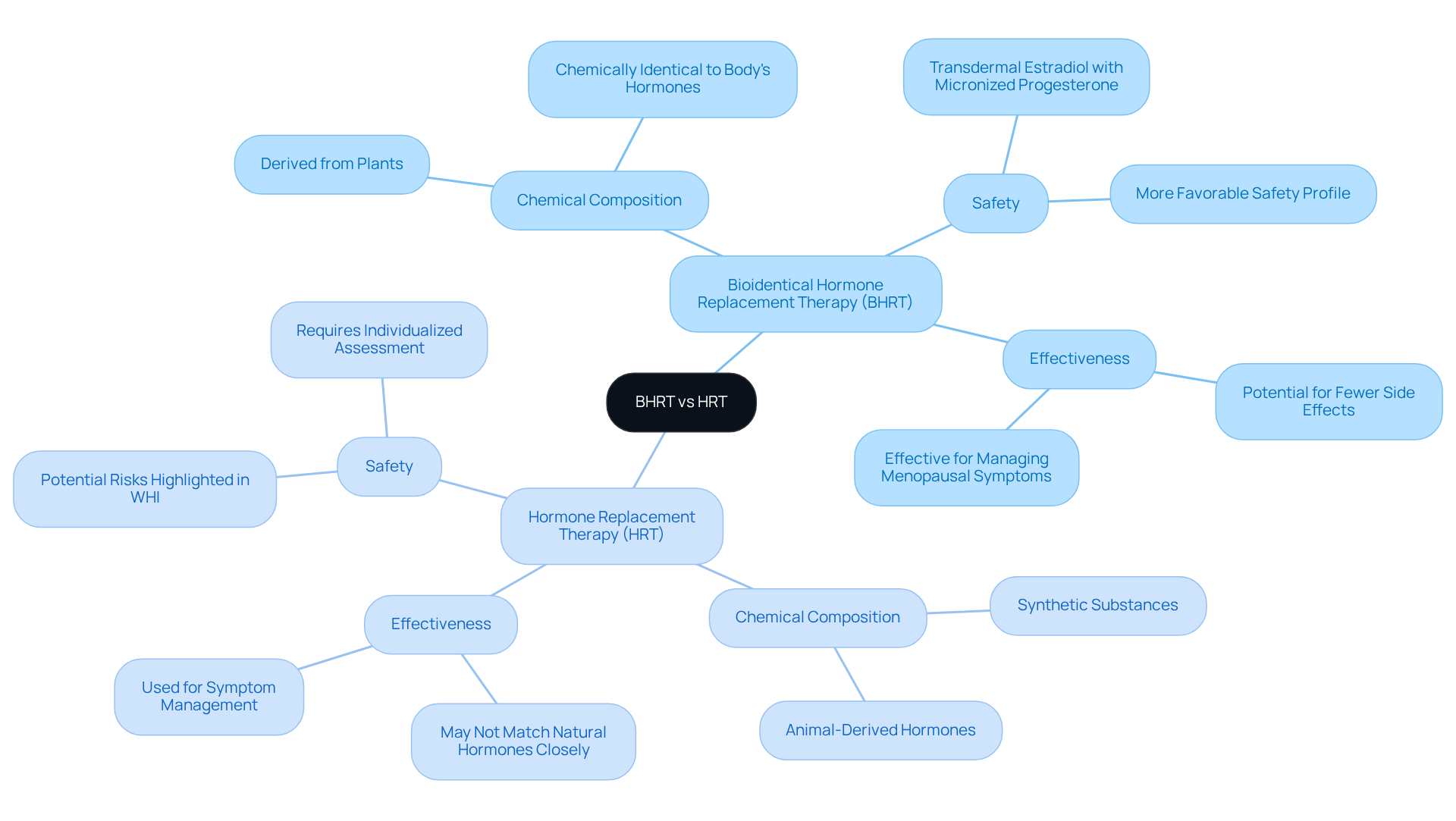
Menopause can bring a host of uncomfortable symptoms, like hot flashes, mood swings, and sleep disturbances. It’s a challenging time, but both BHRT vs HRT are therapies that aim to ease these symptoms. Bioidentical replacement therapy stands out for its personalized approach, allowing for tailored dosages that align closely with your individual hormone levels. This customization may lead to fewer side effects, which is a comforting thought.
Moreover, some studies indicate that bioidentical hormone replacement therapy (BHRT) might offer protective benefits against osteoporosis and heart disease, especially when started within ten years of menopause onset - a concept known as the timing hypothesis. On the other hand, traditional hormone replacement therapy (HRT) has been linked to increased risks of certain health issues, including breast cancer and cardiovascular events, particularly with long-term use. The Women's Health Initiative (WHI) study highlighted these risks, focusing mainly on synthetic hormones that differ significantly from the bioidentical options available today.
In a positive turn, the recent removal of the FDA's black box warning regarding these therapies is a significant step forward, potentially easing concerns for patients about their safety. Understanding these risks, along with the and collaborative decision-making, is crucial as you consider your options. The choice between BHRT vs HRT can profoundly impact your health journey, making it essential to feel supported and informed every step of the way.
Compare Customization and Personalization in Treatment
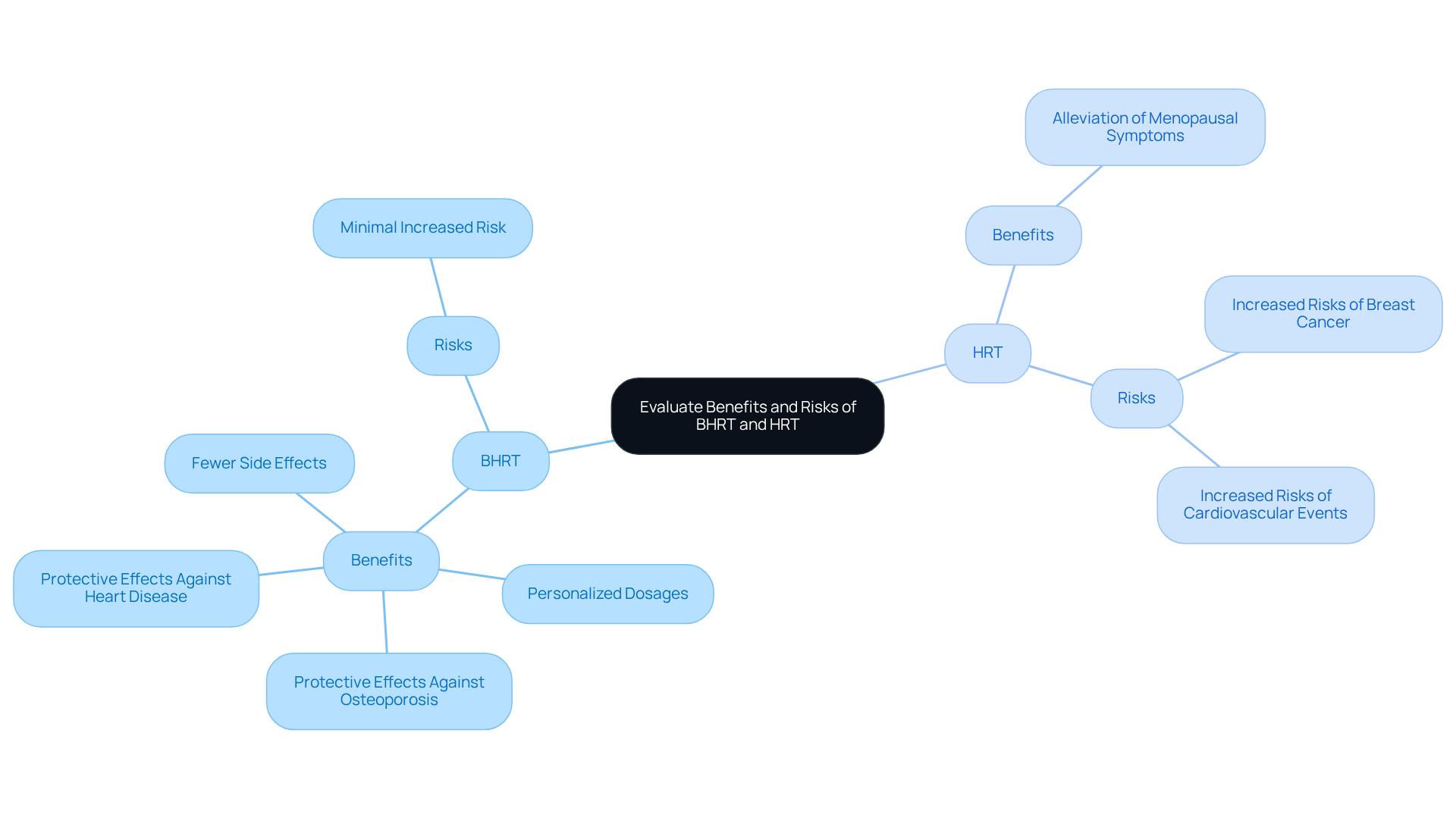
Customization is a key feature that distinguishes BHRT vs HRT. Here, treatment plans are thoughtfully crafted based on thorough testing and individual health profiles. This allows practitioners to create regimens that specifically address each patient's unique hormonal needs. In contrast, the debate of BHRT vs HRT highlights how traditional hormone replacement often relies on standard dosages that overlook personal variations in hormone levels. This one-size-fits-all strategy can lead to less effective results and a greater chance of side effects.
By tailoring hormonal treatment to the individual, BHRT not only enhances treatment effectiveness but also significantly boosts patient satisfaction. This makes it a favored option for those looking for a more comprehensive way to manage their hormones. Recent statistics reveal that about 2 million women in the U.S. received a prescription for hormonal treatment in 2020, highlighting the growing interest in personalized endocrine care. Moreover, experts agree that individualized hormone therapy can lead to better health outcomes, especially when started close to the onset of menopause.
Identify Ideal Candidates for BHRT and HRT
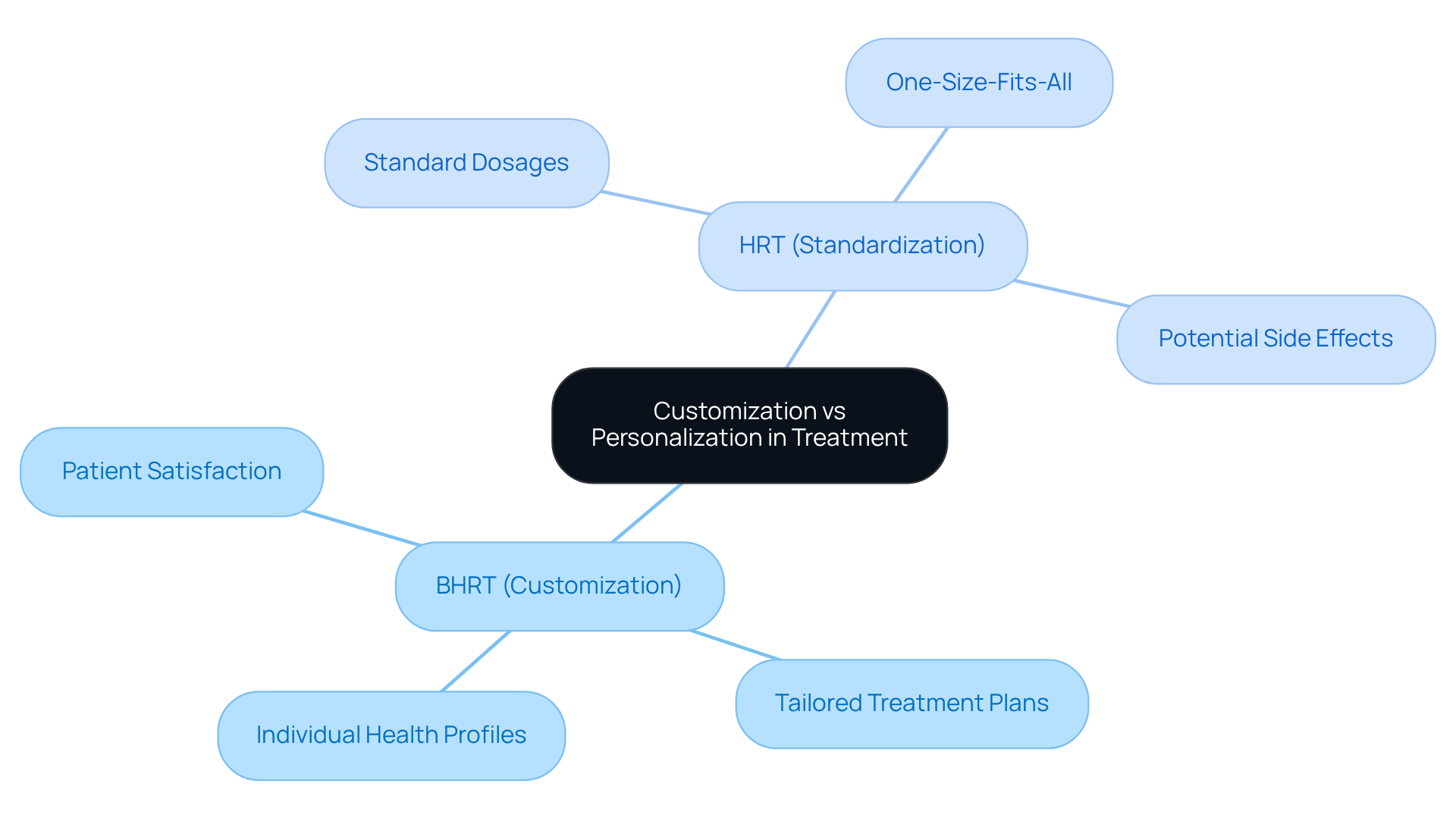
For many women, facing moderate to severe menopausal symptoms can feel overwhelming, especially when lifestyle changes or conventional hormone replacement therapy haven’t provided the relief they desperately seek. This struggle is not just physical; it can deeply affect emotional well-being and quality of life. It’s important to know that you’re not alone in this journey.
When considering treatment options, many seek to understand the for those who have not found success with other therapies. Its formulation is designed to closely mimic the hormones naturally produced by your body, which can lead to a more personalized and effective approach. For women with a history of hormone-sensitive cancers or certain cardiovascular conditions, the discussion of BHRT vs HRT indicates that BHRT may present a safer alternative, associated with lower risks compared to traditional methods.
On the other hand, when considering BHRT vs HRT, traditional hormone replacement therapy can still be a viable choice for women within ten years of menopause, provided there are no contraindications. Understanding these options is crucial. It empowers you to have informed discussions with your healthcare provider, ensuring that the treatment you choose aligns with your unique health circumstances and needs.
Ultimately, the goal is to find a solution that brings comfort and relief, allowing you to embrace this stage of life with confidence and ease.
Conclusion
Bioidentical Hormone Replacement Therapy (BHRT) and traditional Hormone Replacement Therapy (HRT) present different paths for managing hormonal imbalances, especially during menopause. For many women, navigating these options can feel overwhelming. It’s crucial to understand these differences to find relief from menopausal symptoms. BHRT uses hormones that closely mimic what the body naturally produces, which may lead to more effective treatment with fewer side effects. On the other hand, HRT often relies on synthetic or animal-derived hormones, which might not meet individual hormonal needs as effectively.
Throughout this discussion, we’ve highlighted key insights, such as:
- The importance of customizing treatment plans
- Weighing the benefits and risks of each therapy
- Recognizing the value of timely intervention
Research indicates that starting hormone therapy early can significantly lower the risk of osteoporosis and fractures. Additionally, the recent removal of the FDA's black box warning on these therapies is a positive development, encouraging women to explore their options with renewed confidence.
As the dialogue around BHRT and HRT evolves, it’s more important than ever for women to engage in informed conversations with their healthcare providers. By understanding the unique characteristics and benefits of each therapy, individuals can make empowered choices that align with their health goals, ultimately enhancing their quality of life during this significant transition.
Frequently Asked Questions
What is Bioidentical Hormone Replacement Therapy (BHRT)?
BHRT is a treatment designed to alleviate hormonal imbalances using substances that are chemically identical to those naturally produced by the body, such as estradiol and progesterone, which are derived from plants.
How does Hormone Replacement Therapy (HRT) differ from BHRT?
Traditional HRT often relies on synthetic substances or those sourced from animals, which may not match the body’s natural hormones as closely as bioidentical hormones used in BHRT.
What are the potential benefits of BHRT compared to HRT?
BHRT may offer more effective relief from hormonal imbalance symptoms with fewer side effects due to its chemical similarity to natural hormones, while traditional HRT may have a different interaction with the body.
What does recent research suggest about the safety of BHRT?
Recent studies suggest that bioidentical substances, particularly transdermal estradiol combined with micronized progesterone, may present a safer option compared to synthetic alternatives, as highlighted in the Women’s Health Initiative (WHI).
How can starting hormonal treatment early benefit postmenopausal women?
Research indicates that starting hormonal treatment early can reduce the risk of osteoporosis and fractures in postmenopausal women, with those beginning HRT shortly after menopause experiencing a 13% lower risk of fractures.
Why is it important for women to consider the differences between BHRT and HRT?
Understanding the differences in safety, effectiveness, and individual health needs is crucial for women to make informed decisions about their treatment options and to engage with healthcare providers for customized treatment plans.
List of Sources
- Define BHRT and HRT: Core Differences
- Women's Health Initiative Study: What It Means for BHRT in 2026 | Yoo Direct Health (https://yoodirecthealth.com/blog/womens-health-initiative-bhrt)
- New study finds early hormone replacement therapy reduces risk of osteoporosis and fractures for older women (https://aaos-annualmeeting-presskit.org/2026/research-news/new-study-finds-early-hormone-replacement-therapy-reduces-risk-of-osteoporosis-and-fractures-for-older-women)
- BHRT vs Traditional HRT: Which is Safer and More Effective? (https://goldenrosemedspa.com/blog/bhrt-vs-hrt)
- FDA Approves Labeling Changes to Menopausal Hormone Therapy Products (https://fda.gov/news-events/press-announcements/fda-approves-labeling-changes-menopausal-hormone-therapy-products)
- Evaluate Benefits and Risks of BHRT and HRT
- BHRT and Cancer Risk: Modern Evidence vs. Fear (https://navacenter.com/bhrt-and-cancer-risk)
- Hormones for menopause are safe, study finds. Here's what changed (https://npr.org/sections/health-shots/2024/05/01/1248525256/hormones-menopause-hormone-therapy-hot-flashes)
- Women's Health Initiative Study: What It Means for BHRT in 2026 | Yoo Direct Health (https://yoodirecthealth.com/blog/womens-health-initiative-bhrt)
- FDA Updates on Hormone Therapy | Anat Sapan MD Mill Valley, CA California, Illinois, Florida, and New York (https://doctoranat.com/blog/the-fda-just-removed-the-black-box-warning-on-hormone-therapy-heres-what-it-means-for-you)
- I treat menopause and its symptoms, and hormone replacement therapy can help – here’s the science behind the FDA’s decision to remove warnings (https://usnews.com/news/health-news/articles/2026-02-24/i-treat-menopause-hormone-replacement-therapy-can-help-heres-the-science-behind-the-fdas-decision-to-remove-warnings)
- Compare Customization and Personalization in Treatment
- US FDA approves labeling changes to menopause hormone therapies (https://reuters.com/business/healthcare-pharmaceuticals/us-fda-approves-labeling-changes-menopausal-hormone-therapy-products-2026-02-12)
- How the FDA’s Latest Decision Is Changing Hormone Therapy in 2026 - Madison Wellness & Aesthetic Center (https://madisonfamilycare.com/blog/how-the-fdas-latest-decision-is-changing-hormone-therapy-in-2026)
- FDA updates labels on multiple menopausal hormone therapies | Contemporary OB/GYN (https://contemporaryobgyn.net/view/fda-updates-labels-on-multiple-menopausal-hormone-therapies)
- FDA Approves Drug Labeling Changes to 6 Menopausal Hormone Therapy Products | Pharmacy Times (https://pharmacytimes.com/view/fda-approves-drug-labeling-changes-to-6-menopausal-hormone-therapy-products)
- FDA Approves Labeling Changes to Menopausal Hormone Therapy Products (https://fda.gov/news-events/press-announcements/fda-approves-labeling-changes-menopausal-hormone-therapy-products)
- Identify Ideal Candidates for BHRT and HRT
- Who Will Benefit Most from BHRT? Understanding the Ideal Candidates and Age Groups (https://bodylogicmd.com/blog/who-will-benefit-most-from-bhrt-understanding-the-ideal-candidates-and-age-groups)
- Good Candidates for Bioidentical Hormone Therapy: Women's Wellness MD: OB/GYNs (https://womenswellnessmd.com/blog/good-candidates-for-bioidentical-hormone-therapy)
- BHRT vs. HRT: What to know (https://medicalnewstoday.com/articles/bhrt-vs-hrt)
- BHRT vs Traditional HRT: Which is Safer and More Effective? (https://goldenrosemedspa.com/blog/bhrt-vs-hrt)
- seug.com (https://seug.com/blog/who-is-a-candidate-for-bhrt)




